Confirmation
Virtual Influenza-Like-Illness (ILI) Assessments
CPG: Virtual Health
Created: May 13, 2020
Updated:
Author: Chris Michel
Introduction:
Virtual care is healthcare at a distance and many assessments need to be adapted in the absence of a face-to-face interaction1. General ILI assessments may involve using a stethoscope to listen for lung sounds which is not available in virtual healthcare settings. Information will need to be gathered in other ways, such as listening to the patient’s cough, or the audible presence of adverse breath sounds, such as wheezing. As with conventional assessments, determine if the patient is experiencing a particular problem and focus on that area first2.
Essentials3:
-
Set-up: Before initiating a virtual visit, make sure you are set up properly, have access to the patient chart, and any additional information that may be required.
-
Connect: Determine the most appropriate method for communicating with the patient (either phone or video chat). Confirm that your audio and video connections are working properly.
-
Get started: Once you begin the visit, perform a rapid assessment to determine if any immediate interventions are needed. For example, does the patient appear very sick, or are they too short of breath to speak? If so, go directly to asking key clinical questions. If no immediate interventions are required, establish what the patient hopes to gain from the visit (i.e., clinical assessment, referral, reassurance).
-
History: Ask questions to determine a history of the present illness.
-
Examination: Perform a modified physical exam and ask functional inquiry questions.
-
Vitals: The patient may be able to take their own measurements if they have access to vitals equipment at home (i.e., blood pressure monitor, pulse oximeter, scale). Interpret results with caution and use them to support findings in the context of your wider assessment.
-
Decision and action: Based on the follow-up assessment, patients may be discharged from care or referred for a 911 emergency response. Patients with worsening conditions, or those exhibiting red-flag symptoms, should be instructed to immediately call 911 for assessment and conveyance to hospital. Patients whose conditions have not worsened, and present without any red-flag symptoms, may be discharged from care and asked to follow-up with their primary care provider.
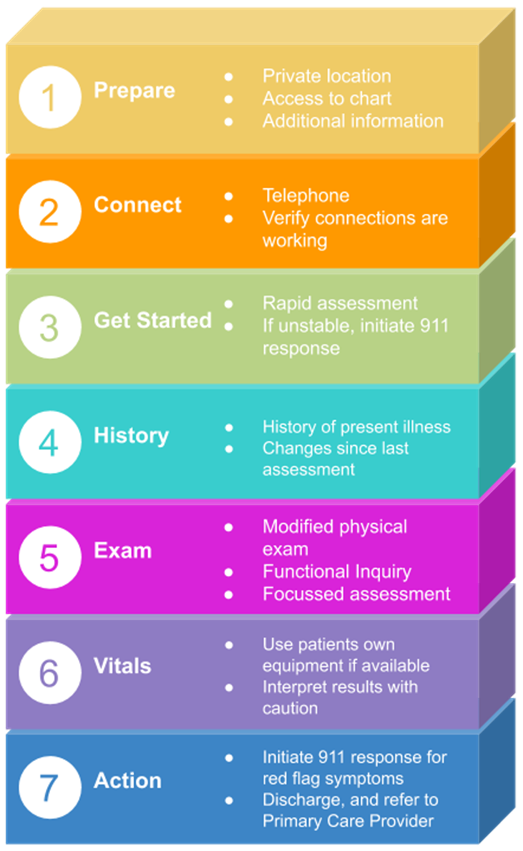
Assessment Overview:
-
Patients who have entered the ILI Clinical Pathway will have been previously assessed by a paramedic and will have met the following criteria:
-
Between the ages of 17 and 60
-
No ‘red flag’ symptoms
-
No single NEWS2 score of 3 and have a total NEWS2 score of 3 or less
-
Meets the paramedic’s clinical judgement for non-conveyance to hospital
-
Consults with CliniCall
-
-
Consenting patients will be contacted by a community paramedic within 24-48 hours of the initial assessment. The goal of the ILI follow-up is to assess for worsening patient conditions, or the new presence of any red-flag symptoms.
-
Patients should be assessed using:
-
The BCCDC COVID-19 Screening Tool
-
Systems based approach
-
Presence or absence of red-flag symptoms
-
Virtual Assessments:
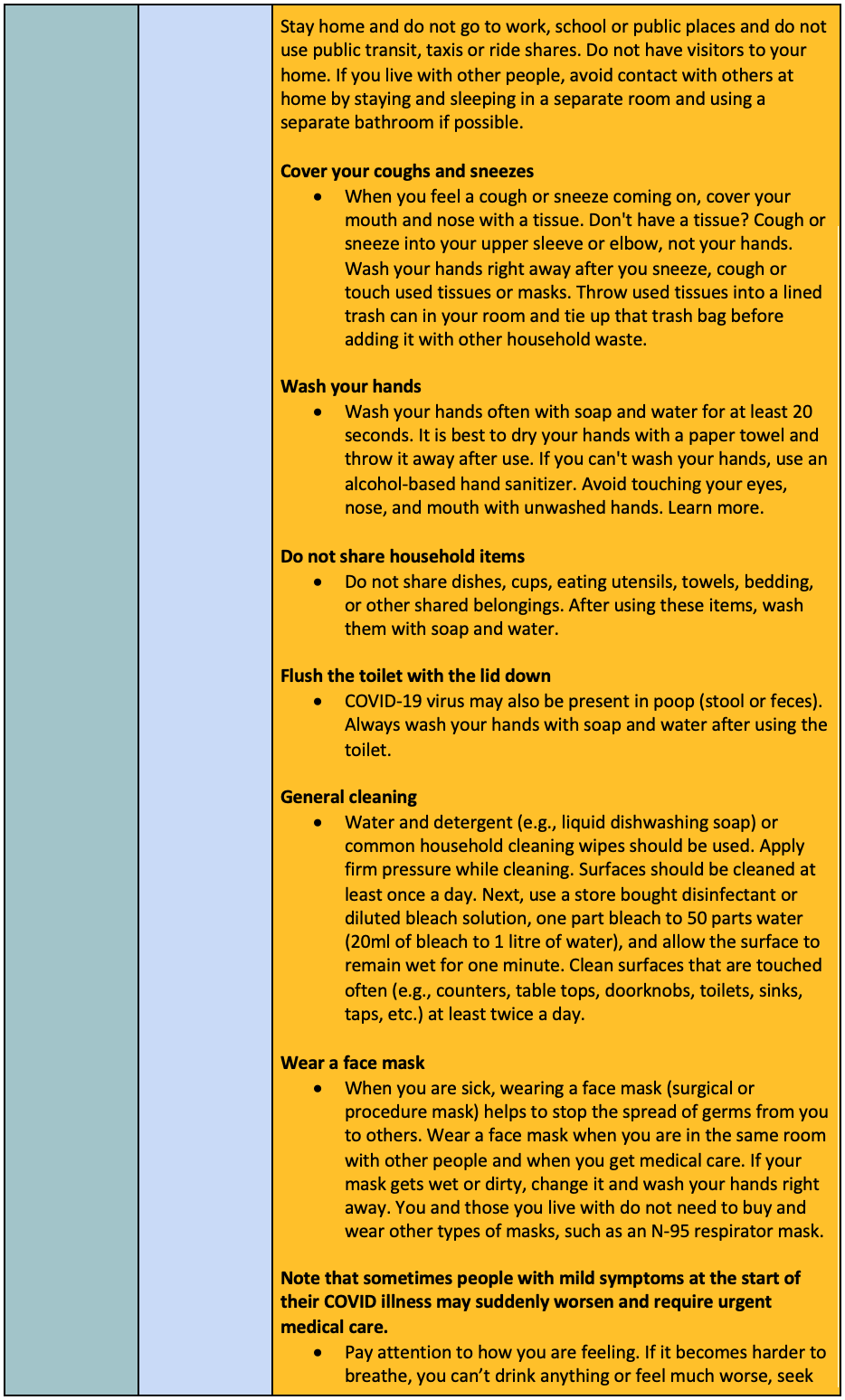
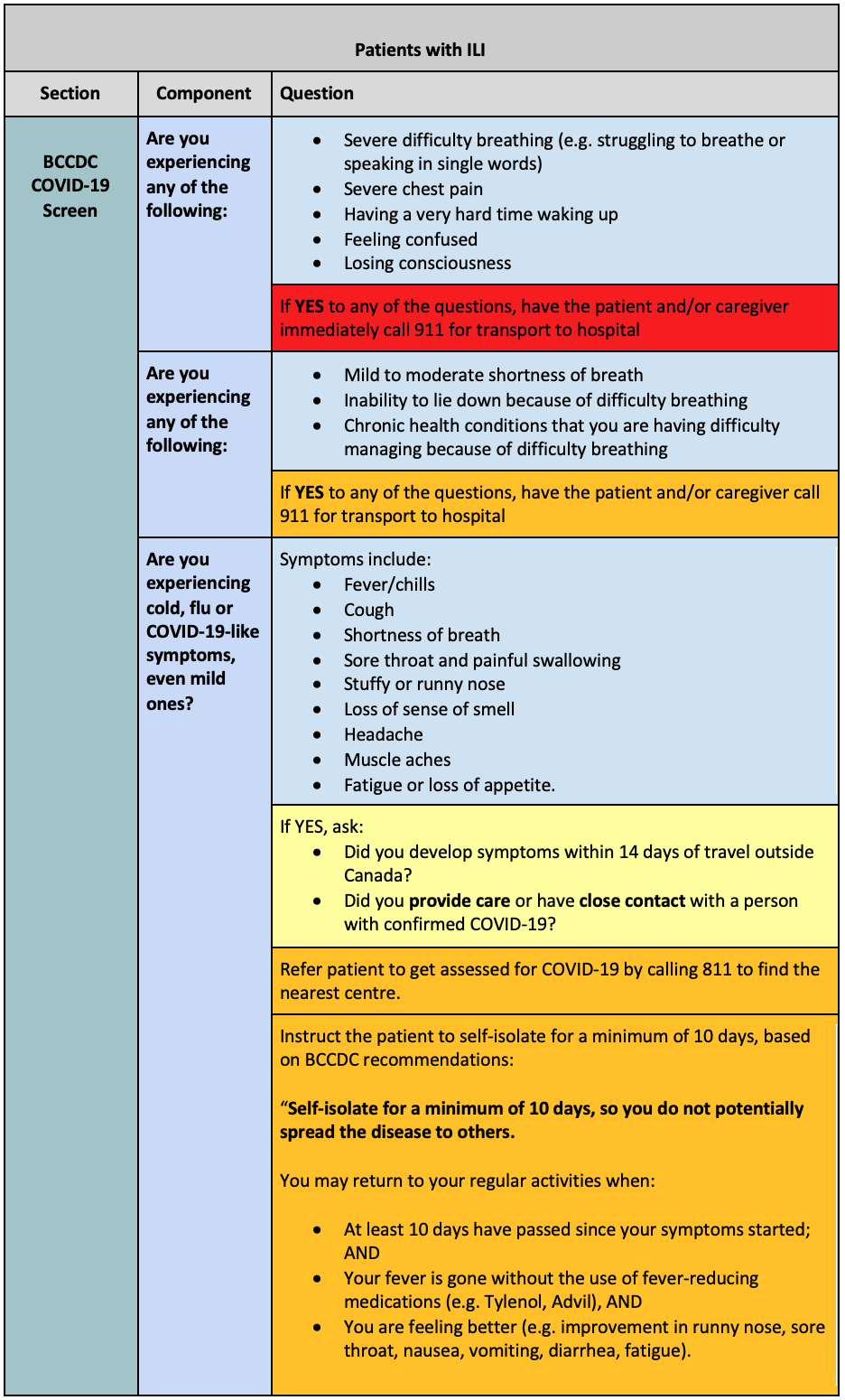

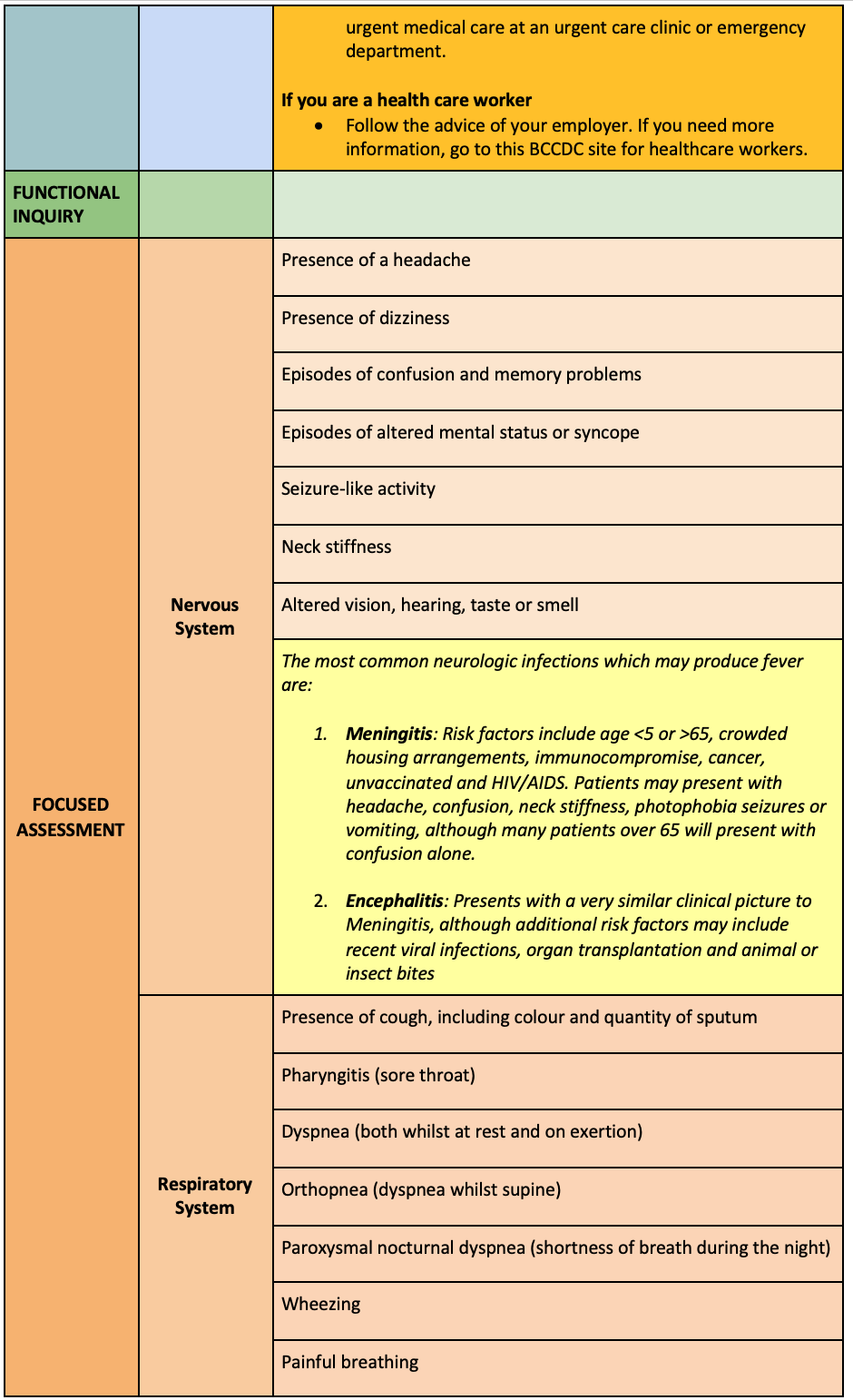
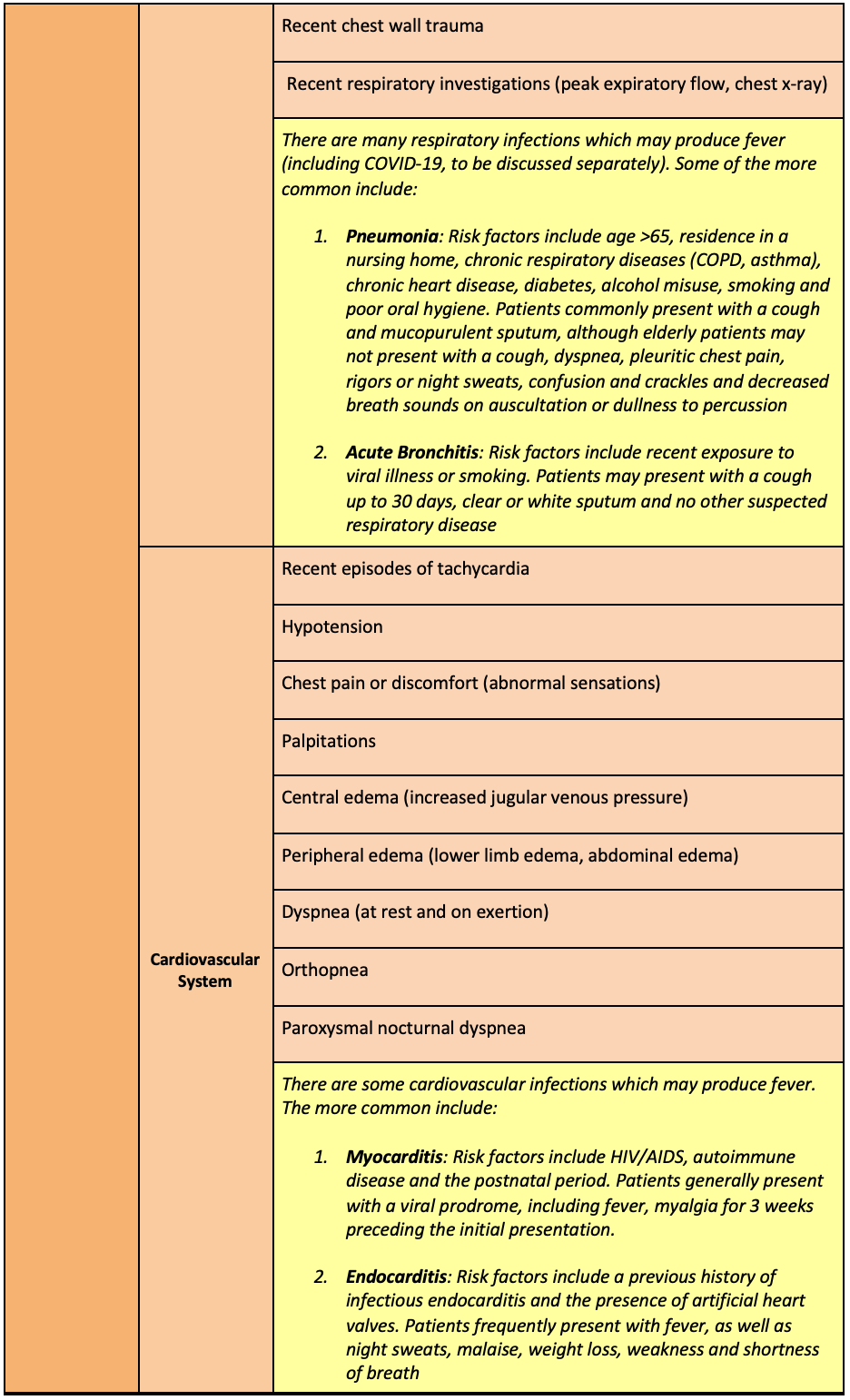
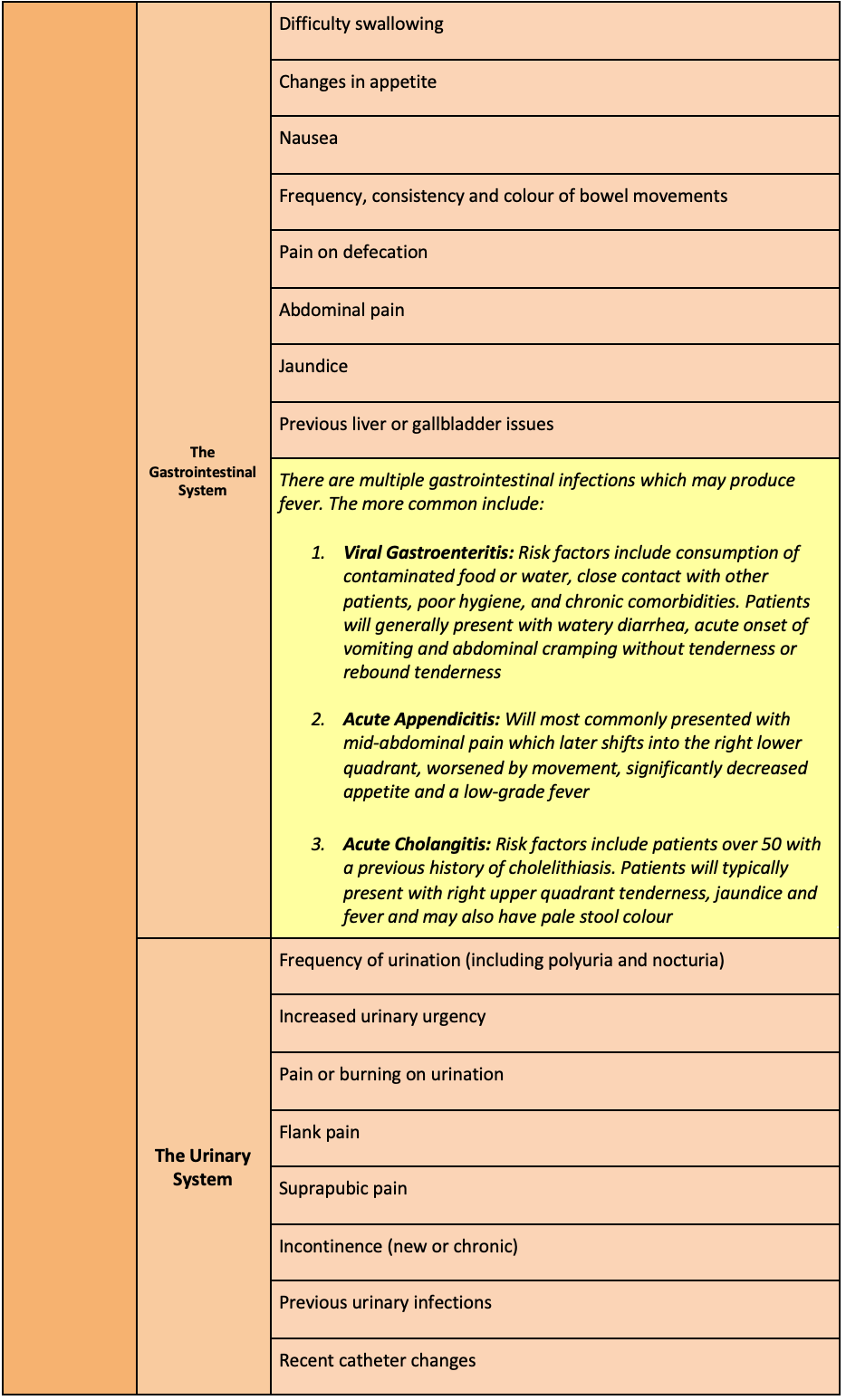
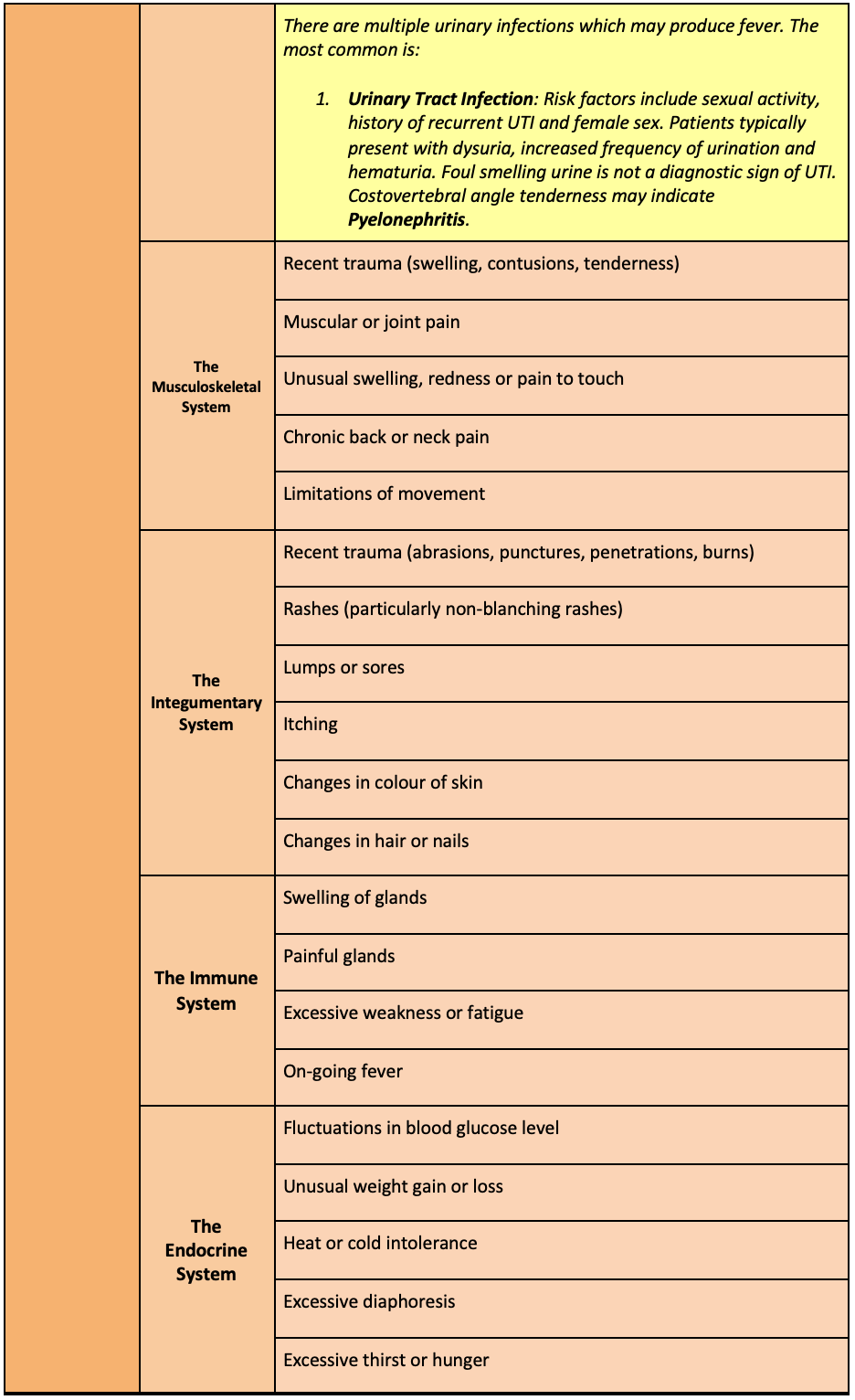

Risk Identification
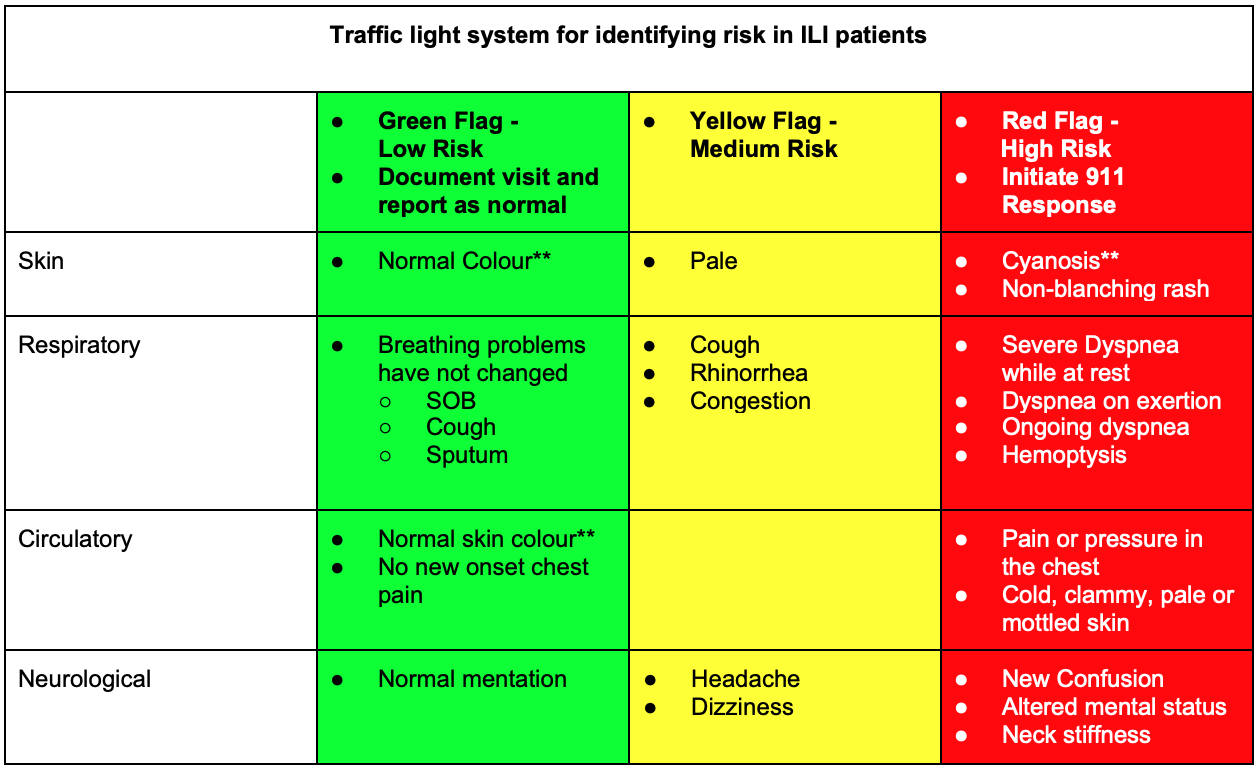 5,6,7,8,9,10,11,12,13
5,6,7,8,9,10,11,12,13
* If able to measure using the patient's supplied equipment
** If able to assess using video conferencing tools
Decision and Action
-
All patients with worsening conditions, or those presenting with any red-flag symptoms, should be instructed to call 911 for emergency assessment and conveyance to hospital.
-
Patients without worsening conditions, and absent of red-flag symptoms, can be discharged and asked to follow up with their primary care provider. Prior to discharge:
-
Patients and/or caregivers should be provided with sufficient discharge advice to be able to identify potential deterioration in condition and act accordingly. This should be documented in the care planning section of SIREN.
-
Patients should be advised to call 911, 811, or the COVID information line (1-888-COVID19) if their condition worsens, or for additional information.
-
References & Further Reading:
- Telemedicine; Researchers from University of Arizona Detail New Studies and Findings in the Area of Telemedicine (Clinical Examination Component of Telemedicine, Telehealth, mHealth, and Connected Health Medical Practices). Medical Devices & Surgical Technology Week [Internet]. 2018 Jun 10;140. Available from: https://ezw.lib.bcit.ca/login?url=https://search.proquest.com/docview/2047463316?accountid=26389
- Martich D. Telehealth Nursing : Tools and Strategies for Optimal Patient Care [Internet]. New York, NY: Springer Publishing Company; 2017. Available from: http://search.ebscohost.com/login.aspx?direct=true&AuthType=ip,sso&db=nlebk&AN=1442257&custid=s5672081
- Greenhalgh T, Koh GCH, Car J. Covid-19: a remote assessment in primary care. BMJ [Internet]. 2020 Mar 25;368:m1182. Available from: http://www.bmj.com/content/368/bmj.m1182.abstract
- Anonymous. Education: Red flag symptoms - Respiratory tract infections. GP [Internet]. 2014 Sep 15;52. Available from: https://ezw.lib.bcit.ca/login?url=https://search.proquest.com/docview/1564433099?accountid=26389
- Schroeder K, Chan W-S, Fahey T. Recognizing Red Flags in General Practice. InnovAiT [Internet]. 2011 Feb 11 [cited 2020 Apr 9];4(3):171–6. Available from: https://doi.org/10.1093/innovait/inq143
- BCEHS ILI/COVID Clinical Practice Guideline. Retrieved from: https://handbook.bcehs.ca/covid-19/covid-tools/ilicovid-clinical-practice-guideline/
- BCEHS – ASTAR-ILI Clinical Pathway Course. Retrieved from: http://learninghub.phsa.ca/moodle/mod/scorm/player.php?a=9746¤torg=articulate_rise&scoid=21647&sesskey=H2A29h6nYE&display=popup&mode=normal